-
- Global AMC MENU
- NEWS
- HEALTH
- PEOPLE
- Introduction
Low recurrence and effective treatment with less pain... High satisfaction among patients with difficult cases
Professor Sa Ra Lee “Leading the way with minimally invasive surgery and contributing to the improvement of patient's quality of life”
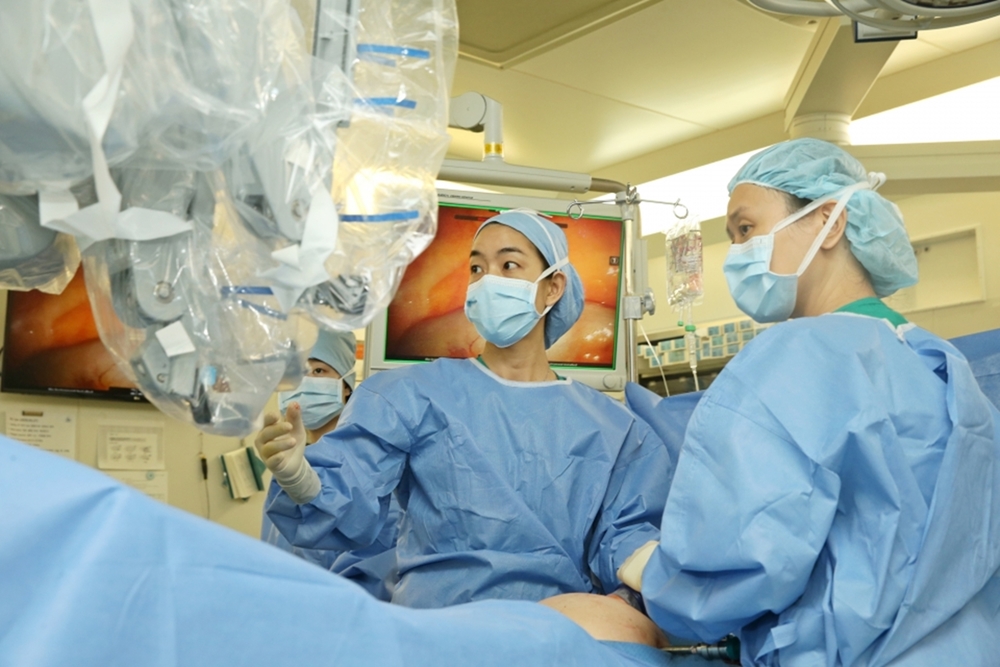
▲ (left) Professor Sa Ra Lee (Obstetrics and Gynecology, Asan Medical Center) performing a robot-assisted sacrocolpopexy
Ms. Lee, a 60-year-old woman, had been experiencing discomfort while walking for the past year as if something was protruding from her groin and getting stuck between her legs. As her symptoms worsened over time, she visited a hospital and was diagnosed with stage 3 bladder and uterine prolapse, which is a considerably advanced stage of pelvic organ prolapse. Despite her relatively young age in her early 60s, active lifestyle, abdominal obesity, and chronic constipation, which are risk factors for the recurrence of pelvic organ prolapse, Ms. Lee opted for robot-assisted surgery, which minimizes abdominal scarring and allows for a quick recovery. After undergoing surgery at Asan Medical Center in late March, she was discharged after only two days of surgery with almost no surgical scars and quick recovery and was able to resume her daily activities.
Pelvic organ prolapse, a condition in which the pelvic muscles supporting the uterus, bladder, rectum, and other organs weaken and allow the organs to slip out of the pelvis, primarily affects women over the age of 60. It causes many inconveniences in daily life, such as walking and urination difficulties and pelvic pain, and therefore, it is important to receive active treatment such as sacrocolpopexy.
In late March, Professor Sa Ra Lee of the Department of Obstetrics and Gynecology at Asan Medical Center became the first in Asia to perform 400 robot-assisted sacrocolpopexy while treating a woman in her 60s who was diagnosed with stage 3 pelvic organ prolapse.
Pelvic organ prolapse is a condition in which the muscles and ligaments supporting the pelvis weaken, causing organs such as the uterus, bladder, and rectum to sag downwards or protrude outwards. It is also known as a 'bottoming out disease.'
The prevalence of pelvic organ prolapse in Korea is 31.7% among those with stage 1 or higher, meaning that 3 out of 10 adult women in Korea suffer from the condition. Particularly, more than half of patients are women in their 60s or 70s, and the number of patients is increasing due to the aging population trend.
Pelvic organ prolapse causes mobility and urinary problems, pelvic pain, and vaginal bleeding, resulting in decreased quality of life. Since symptoms worsen with aging after menopause, active treatment is crucial. Surgical treatment is often necessary as women age, but the recurrence rate is high, with 1 in 3 women requiring reoperation.

▲ Professor Sa Ra Lee (Obstetrics and Gynecology, Asan Medical Center) achieves Asia's first 400 cases of robot-assisted sacrocolpopexy
The most effective and least recurrent treatment for pelvic organ prolapse is sacrocolpopexy, which involves placing a surgical mesh between the vagina and the sacrum, a triangular bone that makes up the posterior aspect of the pelvis.
In the past, sacrocolpopexy was mainly performed through laparotomy or laparoscopy. Laparotomy or open abdominal surgery involves a large incision and a longer recovery time, while laparoscopy has a high risk of complications due to many stitches, resulting in a longer surgery and anesthesia time of 4 to 5 hours and a higher risk of complications.
However, recent advances in surgical robots have made it possible to perform quick and precise surgery through a single incision of around 2.5 cm near the navel. The camera provides high-definition images that can be magnified up to 10 times, allowing for easier dissection and meticulous suturing in tight spaces.
The recurrence rate does not differ significantly between traditional surgery and robot-assisted surgery. However, patients who underwent robot-assisted laparoscopic sacrocolpopexy experienced significant improvements in their quality of life, including reduced pain and faster recovery due to smaller scars, and lower risk of complications due to shorter surgery times.
Professor Sa Ra Lee analyzed 400 patients (average age 57.8 years) who underwent robot-assisted sacrocolpopexy and found that the mean duration of surgery was 1 hour and 20 minutes, and the mean anesthesia time was 2 hours and 30 minutes. This was significantly shorter than the 3 hours and 30 minutes for traditional open surgery and 3 to 5 hours for laparoscopic surgery reported overseas. The average hospitalization stay was 2.05 days.
Most patients (98.6%) had already progressed to stage 3 or 4 pelvic organ prolapse, and 11.4% had undergone other surgeries for pelvic organ prolapse treatment before experiencing a recurrence. The overall recurrence rate of robot-assisted sacrocolpopexy was less than 1%, and there were no recurrences in 213 patients under the age of 60 who are at a particularly higher risk of recurrence.
Professor Sa Ra Lee of the Department of Obstetrics and Gynecology at Asan Medical Center said, "Pelvic organ prolapse tends to have a higher recurrence rate compared to other conditions, but by utilizing the advantages of robot-assisted surgery to perform sacrocolpopexy can significantly reduce concerns about recurrence."
"The satisfaction level of patients who require difficult surgeries such as those who are obese, have severe adhesions from previous surgeries, or are elderly is also very high. I will continue to lead the field of minimally invasive surgery such as sacrocolpopexy and strive to contribute to improving the quality of life for female patients," she added.












