-
- Global AMC MENU
- NEWS
- HEALTH
- PEOPLE
- Introduction
Ms. So Jin Seok, Operating Room Nursing Team

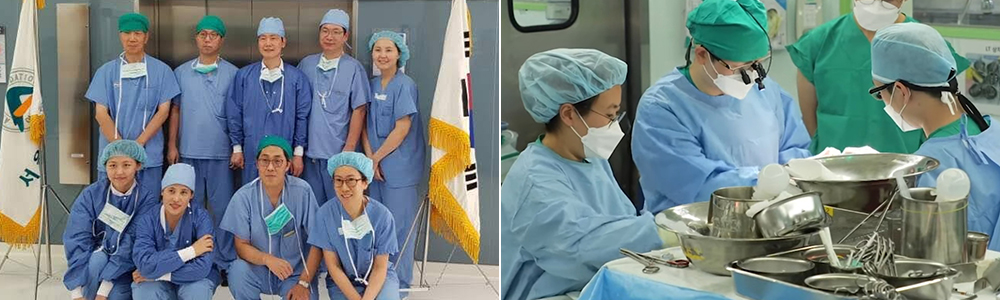
▲ Commemorative photo with medical staff after a conference in Thailand in 2009. Ms. So Jin Seok is the third person from the left in the back row.
▲ Preoperative photo with local medical staff in Vietnam in 2012, ahead of a makeshift surgery. Ms. So Jin Seok is in the middle.
Dramatic narratives persist within the operating room (OR) where transplantations take place. Ms. So Jin Seok, who has worked in Rosette D since 2002, has never experienced a day where the burden of nursing felt trivial. Her responsibilities placed her in constant ‘life and death’ scenarios. In light of these challenges, she now recounts her story, highlighting the unwavering determination and profound pride that flourished amidst the hardship.
How did you feel when you were assigned to Rosette D in 2002?
To be completely honest, I arrived at Rosette D in tears, fully aware of the immense challenges that awaited me. At that time, liver transplantation often exceeded 20 hours in duration. As a nurse assigned to surgery, my work began in the morning and extended well into the following day, leaving me no time even to hydrate myself. Due to the scarcity of trained nurses, we were unable to rotate shifts effectively. Consequently, numerous nurses chose to resign during the first half of 2002. Urgent recruitment campaigns were launched by each Rosette to attract experienced nurses, and it was through such circumstances that I became part of the team.
Transplantations pose significant technical difficulties and entail substantial risks. It typically takes 5-6 years of training before one can assume full responsibility for surgical procedures. Despite the improvements in training conditions, the same holds true today. I was fortunate to receive intensive training within a short period because my assignment coincided with a critical need for nurses.
You must encounter various emotions when witnessing life and death in the operating room
Brain death is the only operation that officially signifies death within the confines of the operating room. In the early days, I found myself deeply empathizing with the families of brain-dead patients, having witnessed such occurrences on multiple occasions. However, it was through a painful personal experience that I truly comprehended the depth of their sorrow. On one occasion, I labored throughout the night, procuring organs from a brain-dead patient, and subsequently moved on to another room to prepare for a pancreatic transplantation. Lost in the demands of my busy schedule, I inadvertently neglected to inform the family of the brain-dead patient and departed for home in the morning. It was while I was asleep, that I received a phone call. Unaware that their loved one had already been transferred to the mortuary, the family had endlessly awaited news at the hospital. The loss of a family member is undoubtedly heartbreaking, and I had inadvertently compounded their pain. I went straight to the funeral, overwhelmed with remorse, and kept crying. The hospital did not reprimand me for my mistake. Instead, necessary changes to prevent such oversights were made to the system as a result. However, no amount of systemic improvements could alleviate the weight of my guilt. Even to this day, I am reminded of that day’s experience when I lecture for nurse refresher training. I consistently emphasize that no matter how busy we are, we must prioritize what truly matters.
Among the heartbreaking scenarios I have encountered, none weigh as heavily on my heart as witnessing brain-dead children. I distinctly recall an instance where a brain-dead child, not yet three years old, received a spare diaper from the grieving mother. I could feel that she sought to ensure her child lacked nothing, although she knew that her child could not make it. Prior to the surgery, my emotions had already been stirred. The entire medical team shared in this sentiment as we delicately removed organs from the fragile body of the tiny child. That very night, as I held my own child, who happened to be the same age as the brain-dead patient, I wept so hard. The thought of enduring a comparable situation, wherein I would be compelled to donate my own child's organs, was an unimaginable anguish.
You also took part in the Asan in Asia project, correct?
Indeed, I had the opportunity to participate in the project aimed at sharing our medical expertise with third countries. Each year, I traveled to nations such as Mongolia, Vietnam, and Qatar. In the initial stages, experienced nurses took turns volunteering their personal time to join the project. During one of my visits to Mongolia, I experienced a physical collapse. The local cuisine proved unappetizing, and the operating room was unbearably hot. Performing complex surgeries with limited personnel, without sufficient time to adapt to the new environment, proved more challenging that I had anticipated. Nevertheless, I witnessed an unwavering sense of duty among everyone involved, even amidst such adverse conditions. As a result, a strong spirit of teamwork naturally flourished.
▲ Commemorative photo taken after makeshift surgery in Qatar in 2016. The first person on the right in the front row is Ms. So Jin Seok.
▲ Performing surgery with Professor DongHwan Jung in 2021. Ms. So Jin Seok is on the left.
Isn’t transplantation highly dependent on the rapport between the nurse and the surgeon?
As transplantation constitutes an exceptionally delicate procedure, the workload and demands associated with it are remarkably high. Surgeons, therefore, cannot afford to wait for a novice nurse to acquire the necessary skills. In my early days, I harbored a deep apprehension towards Professor Shin Hwang of the Division of Liver Transplantation and Hepatobiliary Surgery until I gained some experience. I endured rebukes and suffered blows to my pride in the operating room on numerous occasions. Eventually, I found the courage to address him during a gathering. “Professor, do you realize how disheartening it is? I put tremendous effort in your surgeries.” Opening my heart that day, I discovered that the professor never uttered another word of criticism towards me.
On another occasion, I received an urgent call from the operating room of Professor Ki-Hun Kim of Liver Transplantation and Hepatobiliary Surgery. The patient's condition was rapidly deteriorating, accompanied by profuse bleeding, necessitating the presence of a nurse capable of handling such critical circumstances. Fortunately, the surgery concluded successfully, and later, the professor conveyed his gratitude to me via text, stating, "Thank you for your assistance today." It filled me with immense pride to realize that there was a place where my skills and presence were indispensable. My utmost sense of pride is experienced within the walls of the operating room.
Are there any challenges that still persist in your career?
As I advance in my career, I have been working around the idea that I should have something of my own. Simultaneously, I bear a profound responsibility as a mediator between the surgeons and junior nurses. Furthermore, it is also a pity that the COVID-19 pandemic over the past three years have hindered communication opportunities. I believe it is imperative for me to cultivate greater empathy towards junior nurses and create rapport-building opportunities among the medical staff. My aspiration is to continue contributing to the AMC, where I have dedicated a significant portion of my professional journey.












